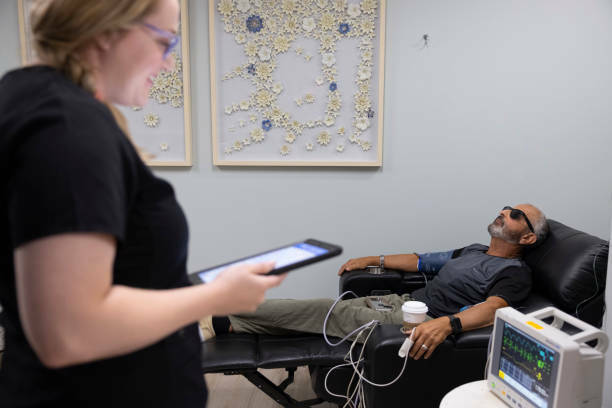
Inside Field Trip Health’s New York City clinic, the vibe is less doctor’s office, a more relaxed spa.
Tucked away on the 11th floor of a nondescript building, you can hear the noise of the busy streets. Instead, this ketamine clinic feels like an oasis of Zen, filled with twinkling lights, greenery, and comfy meditation pillows.
That vibe is part of what drew Chere Sythes, 51, to come back on a chilly Thursday night for another ketamine treatment.
“Some of my friends and colleagues had tried ketamine and other types of psychedelic treatments,” Sithes said. “And talking to them, the stories were hard to believe. But they were people I had known for 20 years, and they seemed like different people. They had a big change.”
Scythes said she first sought ketamine therapy last winter, when she learned that alcohol abuse was taking its toll on her through a series of traumatic events, including her mother’s death, divorce, and, most recently, the loss of her best friend. Over the years, she said, she tried antidepressants, but they didn’t work for her. Meditation and therapy helped but not enough.
“After taking some time off work and meditating a lot I realized I had this deep sadness and this anxiety in my chest,” she said.
Ketamine is a hallucinogen that has been approved by the Food and Drug Administration for decades as an anesthetic but is also used illegally as a party drug. In the past few years, increasing research has found that the drug also works for treatment-resistant depression in some people, leading the FDA to approve a version called esketamine, or Spravato, in 2019. It is an inhaled version that must be administered. A doctor’s office, and it is only approved for people who have failed other treatments.
But in recent years — even before Spravato’s approval — a new industry has emerged: ketamine clinics, which offer the drug off-label either as an infusion or as an injection for a variety of mental health problems. “Off-label” use means that the drug is not specifically approved for those conditions.
At Field Trip, a national chain of clinics that have offered ketamine-assisted psychotherapy for several mental health conditions since 2019, patients first screened to see if they qualify for treatment. If so, patients receive shots of ketamine while they lounge with eye masks as therapists lead them through guided meditation. They also meet with therapists before and after their “trips.”
“Patients say, ‘It changed my life,'” said psychiatrist Mike Dow of the Field Trip Clinic in Los Angeles.
It is not clear how ketamine works in the brain. Dow said he believes it can increase feel-good chemicals like traditional antidepressants, as well as reduce inflammation, and form new neural pathways associated with the ability to create new habits and behaviors.
People also undergo psychedelic experiences that can make them feel spiritual, which in itself can boost their mood, Dow said.
But as the number of new ketamine clinics grows, centers spread across the country, some doctors worry it’s an unregulated industry ripe for danger.
Because the drug has FDA approval, any doctor can prescribe it off-label. The clinics are not federally regulated, but they are subject to the same state laws as other outpatient medical clinics.
Associate professor and president of Stanford University School of Medicine Dr. Smita Das said, “The concern with these clinics popping up is that people are getting treatments that are not well-proven, well-studied, or do not follow any guidelines”. American Psychiatric Association’s Council on Addiction Psychiatry. “My concern is that people who need treatment will spend their money and energy on these ketamine clinics that are not well-proven.”
The treatments can be expensive — from $400 to $800 a session, on average, said Catherine Walker, CEO of Revitalise, a chain of clinics that offer ketamine infusions — and they’re not covered by insurance.
There can also be side effects, including changes in mood and blood pressure, as well as nausea and drowsiness.
Das and Dow say they are also concerned that some clinics may offer the drug without any supervision, which is especially worrisome if the patient has had a “bad trip.”
Only a few small studies have looked at its benefits for other mental health conditions outside of treatment-resistant depression, and the American Psychiatric Association does not offer specific guidelines for its use.
“People rarely experience paranoia or suicidal thoughts,” Das said. “And many of these clinics don’t have mental health professionals. When those mental health concerns pop up, they may not be equipped to respond appropriately.”
Ketamine is also not a cure-all. Not everyone responds to treatment, and it may stop working in some people, says Dr. Subhdeep Virk said.
“It’s very difficult to predict who will respond and how long it will last,” said Virk, who has been treating ketamine patients since 2018. She added that it’s also unclear whether the drug can help with conditions other than treatment-resistant depression.
Lynette Eberts, 66, said ketamine was a lifeline for her. For nearly 40 years, she said, she tried dozens of combinations of antidepressants, electroconvulsive therapy, and other treatments for her severe depression, but nothing worked.
In 2016, before many people had heard of ketamine for depression, her doctor recommended a clinic near where she lives in Raleigh, North Carolina.
“I said, ‘Yes, when and where?'” she said. “I was so desperate to feel better. I thought it was better to try something than to try nothing and take my own life.”
Eberts said each 45-minute infusion felt like a dream, in which he saw vivid colors and shapes. After she had three treatments a week, she said, something began to change.
“I started feeling like I could get out of bed,” she said. “That deep dark cloud of despair began to rise.”
In conjunction with her antidepressants, she has continued ketamine treatments and now receives one every five weeks.
Unlike Ebberts, Scythes does not return to the clinic regularly.
She vividly remembers her first treatment. She saw herself as a little girl, playing in the forest that she loved as a child, and then she saw her mother, who passed away almost 20 years ago.
“How much I love her and how much I miss her, and I feel this unconditional love for her that I never felt when she was alive,” she said. “Once it was over, the deep sadness that had been in my body for so long just disappeared.”